Most people assume candidacy for dental implants comes down to one thing: Do you have a missing tooth? That’s the starting point, sure. But it’s not the whole story, and walking into a consultation without knowing the fuller picture can lead to surprises you didn’t need.
The good news is that more people qualify than they expect. The slightly more complicated news is that “qualifying” isn’t a yes-or-no-it’s a process. Here’s what your dental expert is actually looking at, and why it matters.
Your Jawbone Is Doing Most of the Work
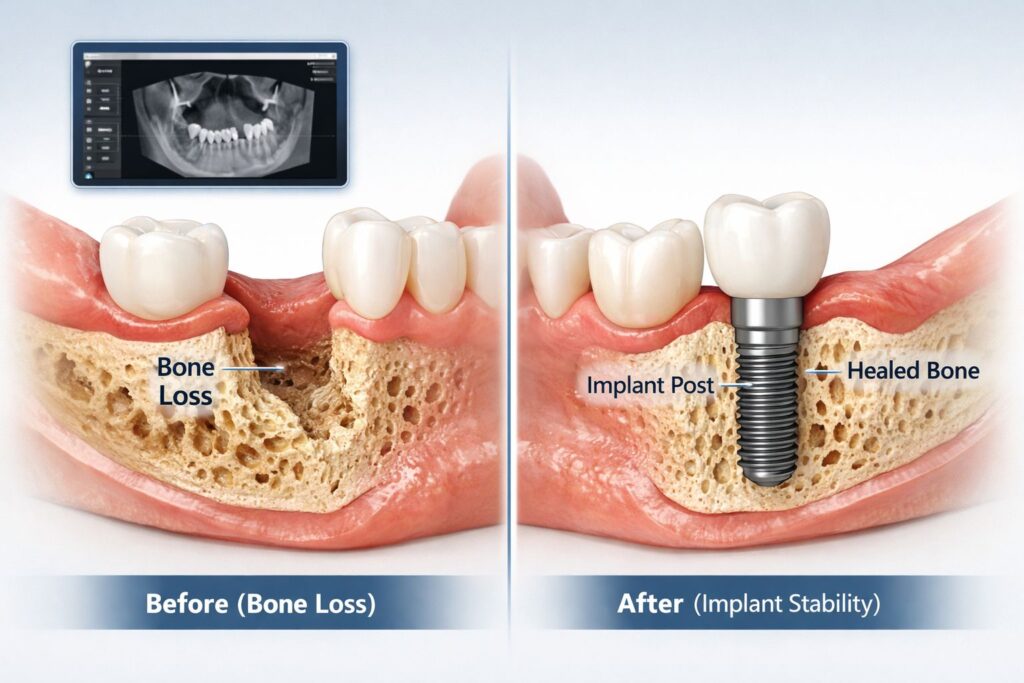
Let’s start here, because bone health is what implant candidacy really hinges on.
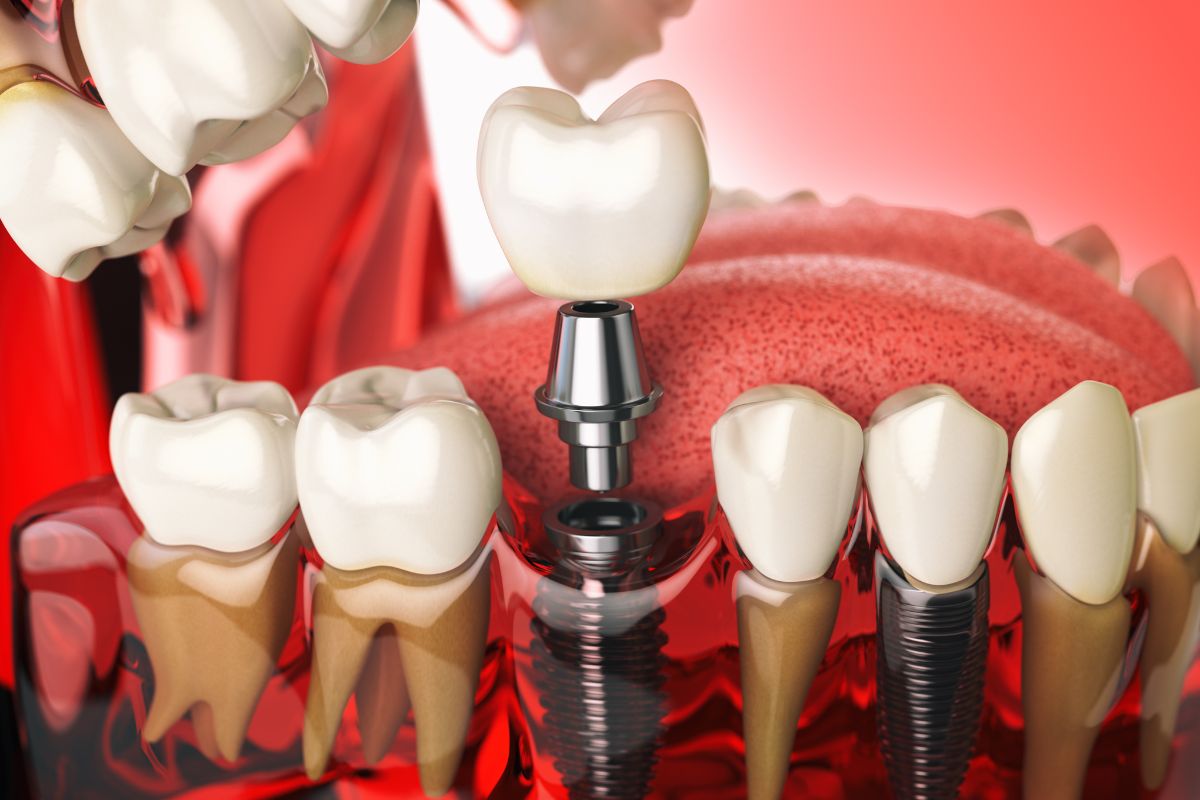
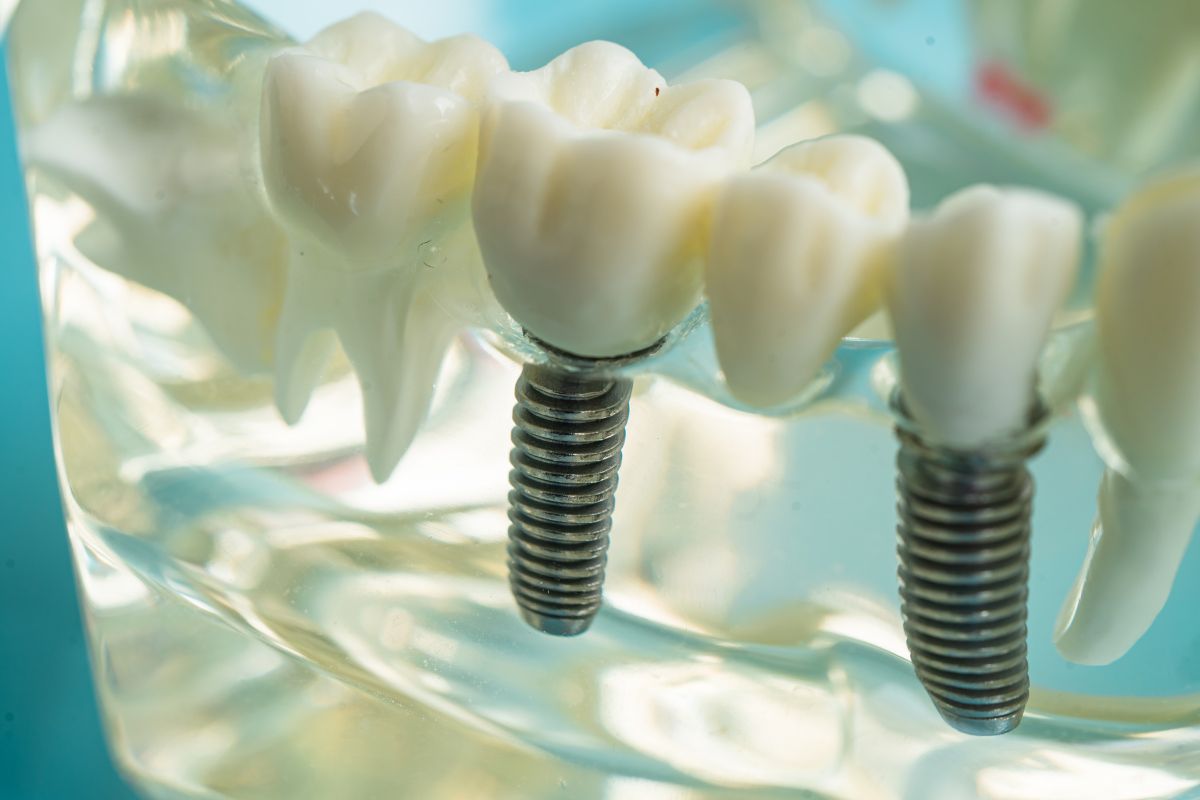
A dental implant is a titanium post that gets placed directly into your jawbone. Over the following months, the bone grows around it, and it’s what makes implants so stable compared to dentures or bridges. For it to work, you need enough bone to anchor the post and hold it under pressure.
Here’s where it gets tricky. Every time you lose a tooth and don’t replace it, the jawbone in that area starts to shrink. Not overnight — but steadily, over months and years. So the longer a tooth has been missing, the more bone volume you may have lost.
That said, bone loss doesn’t automatically take you off the table. Dental implants in Hagerstown at Dr. Cradduck’s office include a full evaluation using cone-beam CT imaging – a 3D scan that provides a precise picture of what’s actually there. If bone grafting is needed to rebuild the site first, that’s a well-established procedure with reliable outcomes. It adds time, but it works.
Gum Disease Is a Dealbreaker – Until It’s Treated
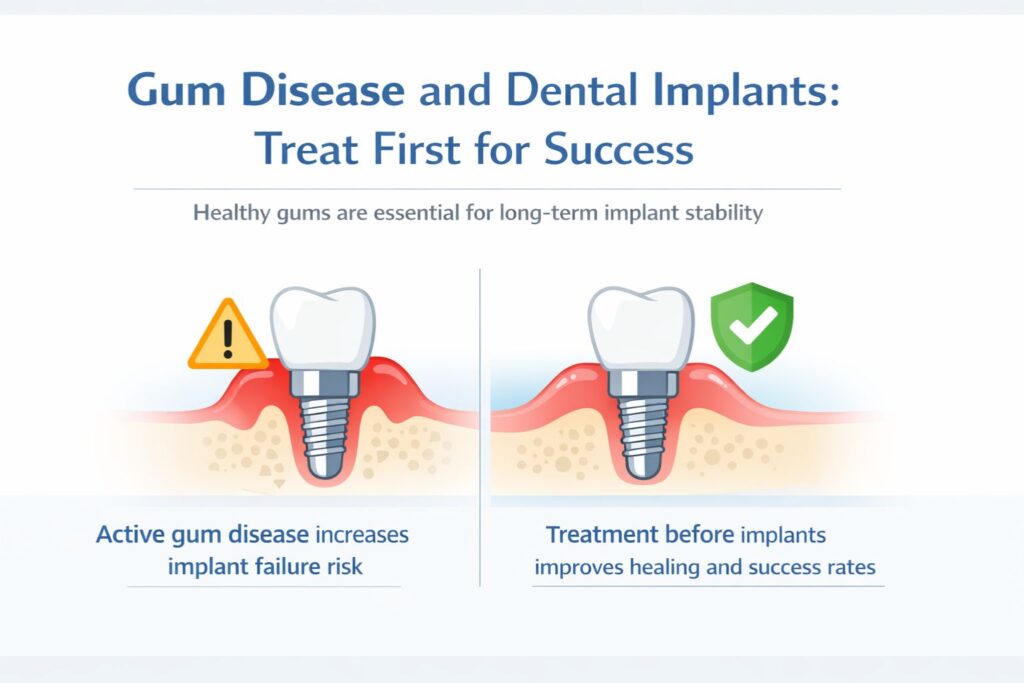
Active periodontal disease and implants don’t mix. That’s not an opinion; the research is pretty detailed on this. When infection is present in the gum tissue or bone, the implant has a much harder time integrating, and failure rates go up significantly.
What this means practically: if your gums need work before implant placement, your dentist will address that first. Some patients see this as a setback. It’s actually the opposite. Treating gum disease before placing an implant is what protects the outcome. A few extra appointments up front are a much better deal than an implant that fails two years in.
Your Medical History Matters More Than You Might Think
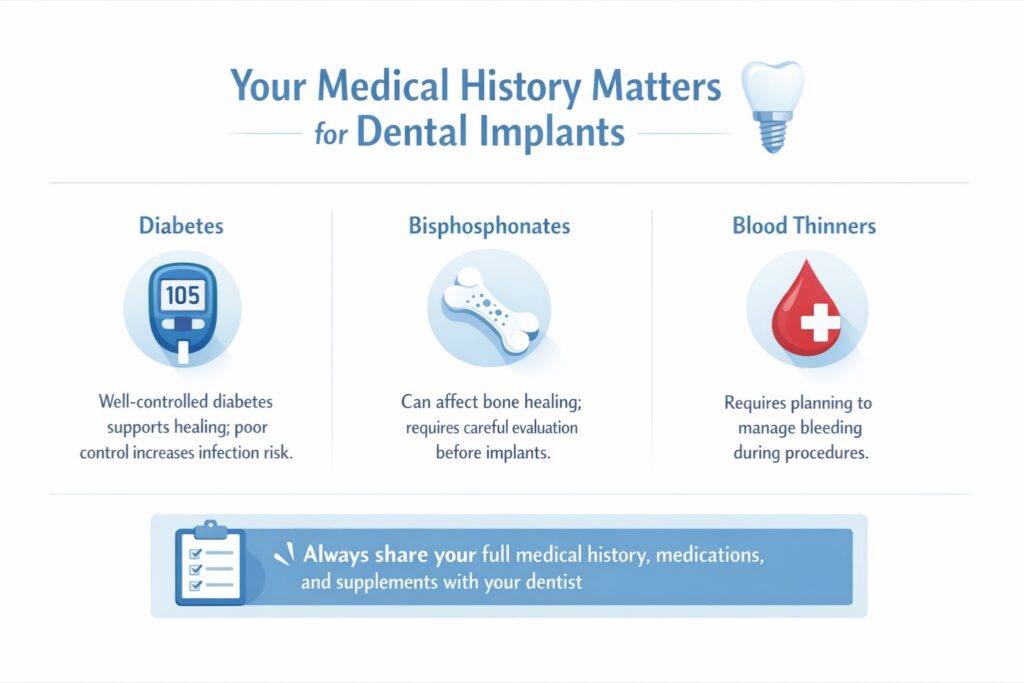
Dental implants are a minor surgical procedure. That means your overall health plays a role in how well you heal, and some conditions require extra planning rather than exclusion.
A few facts worth knowing about:
- Diabetes is one of the most common questions that comes up. Poorly controlled blood sugar impairs healing and increases the risk of infection. But well-managed diabetes? Many patients with diabetes receive implants without issue.
- Bisphosphonate medications (commonly prescribed for osteoporosis) can affect how bone heals around an implant. This needs to be flagged and evaluated carefully. It doesn’t automatically mean no, but it does mean a more thorough conversation is needed.
- Blood thinners affect surgical bleeding and require coordination with your prescribing physician before any procedure. It’s just something that needs proper planning.
The takeaway here is simple: be completely honest with your dentist about your medical history and every medication you take, including supplements. Trying to simplify the list to avoid complicating the appointment usually backfires.
Smoking Is the One Factor That’s Hardest to Work Around
There’s no gentle way to say this — smoking meaningfully increases the risk of implant failure. The data on this is consistent across studies: smokers face failure rates roughly two to three times higher than non-smokers, largely because smoking restricts blood flow and interferes with the healing process after surgery.
If you smoke and you want implants, the conversation isn’t over — but quitting, or at minimum stopping during the healing phase, is something your provider will likely bring up directly. It’s not a lecture. It’s just that the biology doesn’t lie.
Age – Younger Patients Have a Limit, Older Ones Don’t

Implants are not placed in patients whose jaws are still developing. For most people, that means late teens to early twenties, depending on the individual. Before that, the jawbone is still changing shape, and placing a fixed implant during that window creates problems down the line.
On the other hand, patients in their 70s and 80s receive implants regularly. What matters is bone quality and general health, not the number on your driver’s license.
What a Real Candidacy Evaluation Looks Like
At Dr. Cradduck’s Hagerstown practice, candidacy isn’t determined by a quick look and a conversation. It involves imaging, a full health history review, and an honest discussion about your timeline and expectations. Patients across the Hagerstown area, including those coming from Martinsburg, Chambersburg, and Frederick, often come in having done online research and still leave the consultation with a clearer, more accurate picture than they had when they walked in.
That gap between what you read and what’s actually true for your specific mouth is exactly why the evaluation exists.
Dental implants are not for everyone, but they’re for more people than you assume they qualify. Bone loss, health conditions, and even smoking history don’t automatically close the door. What they do is shape the conversation and the treatment plan.
The only way to know is to get evaluated by someone who will give you a straight answer.
Call Dr. Cradduck’s office, Hagerstown Family Dental, to schedule your implant consultation.
People Also Ask
It varies, but most patients complete the full process in three to six months. Cases requiring bone grafting take longer—sometimes 9 to 12 months in total. Your provider will give you a realistic timeline after your initial evaluation, based on your specific bone condition and healing rate.
Often yes, but long-term denture wear typically comes with significant bone loss underneath. That bone loss needs to be assessed before anything else. Some patients need grafting first; others have retained enough bone for implant placement without it. A 3D scan tells the real story.
The procedure is done under local anesthesia, so you shouldn’t feel pain during placement. Soreness for a few days afterward is normal and, in most cases, manageable with over-the-counter pain relief. Most patients say it was considerably less uncomfortable than they anticipated.
Sometimes. In straightforward cases, implants can be placed immediately after extraction or within a few weeks. In others, when infection is present or bone loss is significant, waiting several months for the area to heal is the safer approach. Your provider will assess which applies to you.